The Sequence 3/3-3/9
Hijacked Highways: Cancer's Use of Neural Pathways

Hijacked Highways: Cancer's Use of Neural Pathways
This study discusses the relationship between neurons and pancreatic cancer progression. The researchers studied relationships between the nervous system and pancreatic cancer and identified interactions that in many cases promote tumor growth and survival. Although previous studies have shown that a substantial network of nerves is integrated into pancreatic cancer tumors, it was previously unclear what molecular interactions between the nerve cells and cancer cells take place. This study expanded the scope by molecularly examining the nerve cells in both healthy tissue and pancreatic cancer in mice.
What did the study find about the role of nerves and cancer progression?
Let’s start with understanding the body's neural network and how that relates to some types of cancer, including pancreatic cancer. The Peripheral Nervous System (PNS) is a crucial component of the body's neural network, bridging the gap between the central nervous system (CNS) and the external environment. It encompasses clusters of neuron cell bodies called ganglia. In some cancer cases, nerve fibers project from nerve cells in the ganglia directly into the tumor.
After analyzing individual neurons found in pancreatic tumors in mice, the researchers found that the tumors reprogram the neurons for their own benefit. At that point, gene expression in the tumor is increased or decreased, resulting in a tumor-specific gene signature. The effect was evident even after isolating the tumors outside the body: When scientists re-implanted pancreatic cancer cells into the mice they had been removed from, the resulting secondary tumors grew twice as large as those of mice that had been transplanted with cancer cells for the first time. The fact that these types of tumors are able to reprogram nerve cells ultimately renders them more aggressive and harder to treat.
How does this affect individuals with cancer?
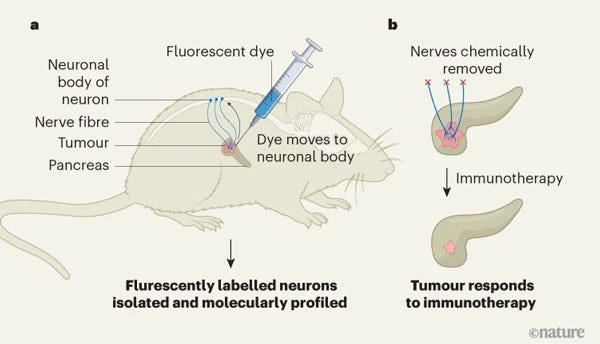
Chemically removing the nerve fibers that promote the growth of pancreatic cancer can make these tumors more responsive to immunotherapy (Nature News & Views; Nature Briefing: Cancer Newsletter February 27, 2025)
In addition to studying how nerve cells affect cancer progression, the group studied a potential cancer treatment that suppresses nerve function. They exposed the tumors to a targeted neurotoxin, which blocked the neural connection to the pancreatic tumor. Turns out, after the neural connections were blocked, the tumors became more sensitive to the checkpoint inhibitor nivolumab and the tumor mass shrank. Overall, tumors became one-sixth of the mass of those in the control animals. According to Simon Renders, first author of the publication, "By blocking the nerves, [we] were able to convert an immunologically cold tumor into one that was sensitive to immunotherapy".
The team took this a step further by combining the technique above with the drug nab-paclitaxel, a component of standard chemotherapy for pancreatic cancer that works by inhibiting cell division and also affecting sensory nerves. When the tumor was completely cut off from its neuronal connections using the neurotoxin to switch off the sympathetic neurons and the sensory nerves were blocked by treatment with nab-paclitaxel, the combination had a complementary effect that reduced the tumor mass by more than 90 percent.
What’s the takeaway?
Researchers studied the network of nerves within tumors, which function like its own communication network. They then observed what happened after the tumors were injected in mice with and without prior pancreatic cancer. They found the cancer cells were actually hijacking these nerves, changing their function to help the tumor grow faster and become more aggressive. The study confirmed that even when they took the tumor out of the body, this "rewiring" effect stayed, making the cancer even harder to fight when it came back. Additionally, blocking nerve function with the use of a special neurotoxin and a chemotherapy treatment inhibited cancer growth and increased the sensitivity of tumor cells to certain chemotherapies and immunotherapies. As nerves are active players in helping pancreatic cancer thrive, pancreatic cancer cells may be susceptible to new treatment options that disrupt their growth by inhibiting neural activity in the future.
https://pubmed.ncbi.nlm.nih.gov/39961335/
https://www.ninds.nih.gov/health-information/public-education/brain-basics/brain-basics-life-and-death-neuron
https://app.jove.com/science-education/14920/peripheral-nervous-system-ganglia-and-nerves
https://www.nature.com/articles/d41586-025-00501-9
https://www.news-medical.net/news/20250217/Pancreatic-cancer-reprograms-nerve-cells-to-fuel-growth.aspx